
Updated May 1, 2020
Non-narcotic pain medications and therapies are growing in importance as we address the opioid epidemic. Treating pain without opioids is becoming increasingly common. More doctors and patients are turning to non-narcotic pain meds and prescribing alternative therapies to treat chronic pain. This article will discuss the many different ways for treating pain without opioids. First, let’s identify the opioid pain medications that we want to reduce.
This is a list of the most common narcotic pain medications used today. The consequences of their widespread use has been deadly and it’s essential that we continue to find ways to reduce our reliance on these medications to manage pain.
Codeine
Fentanyl
Hydrocodone
Vicodin
Demerol
Morphine
Oxycodone
Percocet
Methadone
Hydromorphone
Second, let’s take a look at common non-opioid pain medication used in place of these narcotics to treat pain without opioids.
Some of the most common non-narcotic pain meds are:
Acetaminophen (Tylenol)
Ibuprofen (Advil)
Naproxen Sodium (Aleve)
Aspirin (Bayer)
Gabapentin (Neurontin)
Corticosteroids (Prednisone)
Tricyclic Antidepressants (Amitriptyline)
Topical Agents (Lidocaine)
As you can see, there are many different types of non-narcotic pains meds used for treating pain without opioids. The specific use of each of these medications will be discussed in more detail later in this article.
Two of the most powerful non-narcotic pain killers are IV versions of the OTC pain meds acetaminophen and ibuprofen.
Ofirmec is IV acetaminophen, and is used for managing mild to moderate pain. IV acetaminophen has also been shown to decrease opioid consumption after major surgery by nearly one-third compared with placebo.
Caldolor is IV ibuprofen used for management of mild to moderate pain to eliminate, or reduce, opioid pain medication. Similar to IV acetaminophen, studies have shown IV ibuprofen decreases pain scores and opioid usage.
These powerful non-narcotic pain killers come with their own side effects. The most common side effects are developing kidney or liver problems. They can also cause severe allergic reactions with hives, difficulty breathing, swelling of your face, lips, tongue, or throat.
While there are a time and place for opioids, other pain management techniques are available to help reduce pain without the fear of overdose or addiction. Some of the reasons to consider treating pain without opioids include:
It reduces the risk of overdose
Opioids do not address the source of the pain
Opioids do not increase function
Opioids may increase pain and pain sensitivity over time (doctors call this condition enhanced pain sensitivity)
Opioids don't relieve neuropathic (nerve) pain
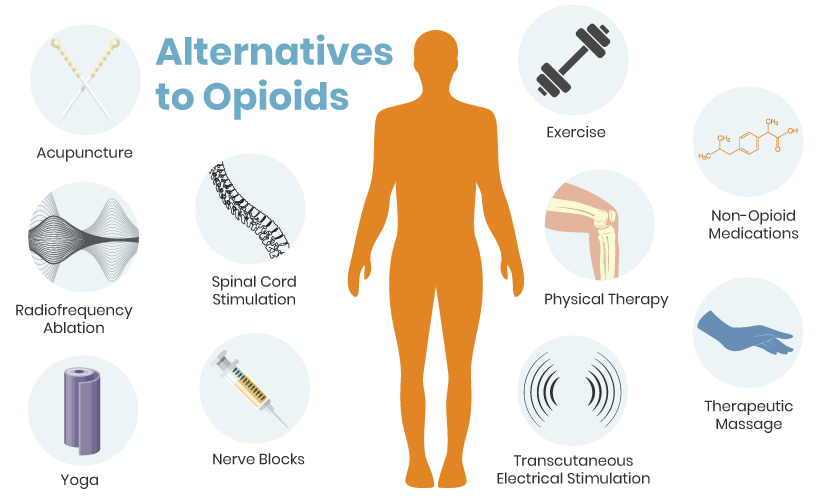
An estimated 20 percent of Americans experience chronic pain.1 There are many alternatives to treating pain without opioids. Frequently, a combination of pain-relieving techniques can help reduce reliance on opioids for managing pain.
If you or a loved one currently takes opioids for pain management, consider speaking to your physician about potential non-opioid treatment options. By working with your doctor and exploring new ways of relieving pain, you may find relief without using opioids.
Acupuncture is a traditional Chinese medicine that involves inserting small, thin needles into key areas of the body to re-direct energy flow in the body. Several studies suggest that acupuncture works particularly well at addressing chronic back and neck pain, knee pain, and headache. There is also some evidence to suggest that acupuncture may help prevent migraines.
Some people don’t like the idea of acupuncture because they’re afraid of someone sticking and leaving needles in their bodies. However, the needles are very small and thin. They aren’t meant to inflict pain, but instead, they relieve pain by releasing endorphins, the body’s natural pain-killing chemicals, and work to improve an overall sense of well-being.
Exercise involves moving, stretching, and engaging in physical activity. Though it may seem counterintuitive, exercise can help some people address chronic pain. Exercise helps maintain a healthy weight, which helps to reduce pain related to conditions like arthritis. Also, exercise helps to relieve stress and anxiety while also releasing chemicals in the brain called endorphins. These are feel-good chemicals that can help reduce pain naturally and increases a sense of well-being.
The Cochrane Database of Systematic Reviews conducted a review of studies about exercise and pain relief.1 They included 21 studies that enrolled more than 35,000 participants. Some of the pain-related conditions they studied included low back pain, rheumatoid arthritis, spinal cord injury, and patellofemoral (knee) pain.
Researchers found that exercise helped to reduce pain severity and improved physical function in people with chronic pain. Those with chronic pain who engaged in exercise also reported an improved quality of life compared to those who did not exercise.
It’s important to understand that some people may have medical conditions that prevent rigorous exercise. It’s always important to talk to your doctor before starting an exercise program if you have concerns about physical ability. Doctors may be able to suggest adaptive exercises or low-impact movements that would work better for you.
Nerve blocks are a non-opioid pain treatment approach where a doctor injects a local anesthetic into the skin and around nerves that are responsible for the pain. While doctors can’t block all nerves, they can typically block abdominal, knee, back, and shoulder pain. Sometimes, doctors will insert special catheters (small, thin plastic tubes) that can deliver continuous amounts of a local anesthetic to provide longer-lasting pain relief.
Opioid medications like morphine, fentanyl, and hydrocodone aren’t the only medicines that can relieve pain. There are over-the-counter(OTC) medications that provide pain relief. The benefit of these medicines is that they don’t have the addictive potential of opioids. While it is possible to overdose on some OTC medications, the amount you’d have to take is extremely high.
Examples of non-opioid medications used to treat pain include:
Ibuprofen (Advil, Motrin)
Acetaminophen (Tylenol)
Aspirin (Bayer)
Naproxen Sodium (Aleve)
These medications often work to relieve inflammation and reduce pain in the body. They’re inexpensive and usually available as generic options. When used in combination with other treatments, like physical therapy, non-opioid medicines can effectively help manage pain.2
Corticosteroids act like hormones you produce naturally in your adrenal glands. Corticosteroids lower inflammation in the body and reduce immune system activity. Both these effects can help with non-narcotic pain management. These drugs are used to treat rheumatoid arthritis, lupus, and Addison’s disease. Corticosteroids are taken in several ways:
By mouth
By inhaler or nasal spray
Topically
By injection
Corticosteroids have many potential side effects and need to be monitored closely by your doctor.
Antidepressants have been found to be effective in treating many different types of pain, including:
Multiple Sclerosis
Diabetes
Shingles
Arthritis
Migraines
Fibromyalgia
We don’t know exactly how these non-narcotic drugs control pain, but it is thought that they might reduce pain signals in the nervous system. Tricyclic antidepressants affect two chemicals in your body, serotonin and nor-epinephrine. Serotonin and nor-epinephrine reuptake inhibitors (SNRIs) affect those chemicals. The SNRI duloxitine (Cymbalta) is the approved for treating pain.
Gabapentin (Neurontin) is an anticonvulsant used to control seizures, but it has been found to control some types of pain. It’s also used to treat headaches, diabetic neuropathy, and fibromyalgia. It’s also a sedative used to treat many other conditions. Gabapentin is one of the most prescribed non-narcotic medication because of this versatility.
Local anesthetics numb painful parts of the body for short periods. Lidocaine patches are one of the most commonly used local anesthetics to treat pain without opioids. Aspirin creams are another type of topical agent that block pain causing substances in the body. Counter-irritants, like BenGay and Vicks Vapor Rub, irritate your nerve endings to distract your brain from other pain.
Physical therapy is the use of exercises and equipment like whirlpools, massage, and ultrasound therapy to help stretch and strengthen muscles and tendons in the body. Physical therapy can help build up muscles around injuries, so there is less demand on the injured area.
Physical therapy also helps address what’s causing pain in the first place. By rehabilitating an injured part of the body, a physical therapist can teach ways to improve overall functioning. This education has the power to help a person feel better long-term.
This approach involves using radio waves to relieve pain. To do this, a doctor will insert a thin needle near the nerve sending pain signals to the brain. They then use electric current to damage or destroy the nerve. This will prevent the nerve from transmitting pain signals for some time.
If the approach sounds similar to nerve blocks, it is. However, according to the American Society of Anesthesiologists, using radio waves can last up to a year.
Spinal cord stimulation is a special device that doctors can implant near the spinal cord. The device itself is in the lower back and has special wires that go to the spinal cord. A special remote control can be used by the person when pain sensations occur. The spinal cord stimulator releases signals that help to “interrupt” traditional pain signals. Instead of feeling a sharp or stabbing pain, they may instead feel a tingling sensation.
In addition to treating problems like back pain, spinal cord stimulation also helps to reduce symptoms in people with peripheral neuropathy, which is a common source of pain and numbness in people who have diabetes with nerve damage.
Therapeutic massage involves using the hands to knead and rub the skin to help relieve muscle tension. Other benefits of therapeutic massage include:
Reducing joint pain
Relieving stress
Reducing anxiety
Some researchers think that therapeutic massage helps to reduce pain by stimulating the surrounding nerves that aren’t transmitting pain signals.3 Basically, the massage and stimulation to healthy nerves drown out the signals of pain, resulting in an overall improvement in well-being.
Several studies have shown the benefits of massage for those with chronic pain. A 2014 study published in the Annals of Family Medicine found that hour-long massage sessions two to three times a week helped to relieve chronic neck pain when compared to shorter massage sessions or no massage at all.3
There are many different types of massage. Sometimes, a person may be afraid the massage will be too “deep” or strenuous on their body. That’s why doctors recommend finding a licensed massage therapist that can help a person identify the best approach to massage with consideration to overall health and pre-existing medical conditions. If there is an active or inflamed area of skin, the massage therapist should know to avoid that area of skin to prevent the further transmission of the infection.
Transcutaneous electrical nerve stimulation therapy involves using special devices that send out low-voltage electrical signals. The device is typically worn and is called a TENS unit. The device has small electrodes on it that can transmit electricity to the skin.
Doctors are the first to admit, they don’t know exactly why TENS units work. They think that the therapy may stimulate the feel-good chemicals called endorphins and that it interrupts pain signals between the brain and body.
Yoga is a therapeutic approach that involves engaging in a series of stretching exercises. Yoga practitioners also commonly engage in breathing exercises to focus the minds while bending and stretching in different poses.
There are many options to participate in yoga, including taking a yoga class at a gym, exercise studio, or community center. There are also a variety of yoga videos available on streaming sites and YouTube that anyone can watch at their home. This makes yoga a low-cost option to relieve chronic pain. Typical yoga sessions include deep breathing and moving through several different poses.
Yoga doesn’t have to mean a person can bend and twist like a pretzel. A lot of different adaptive yoga positions are available for people of all movement abilities. Some people can even perform yoga from a seated position, which is very helpful for those with chronic pain who are wheelchair-bound.
According to the Harvard University Press, several studies support the use of yoga in treating chronic pain.4 For example, an analysis of 17 studies found yoga helped improve daily functioning for patients with fibromyalgia with osteoporosis-like symptoms and back pain. Another study found that weekly yoga sessions helped improve mobility and reduced pain in people with chronic lower back pain.
Cognitive-behavioral therapy (CBT) is a therapy approach where a person learns how to recognize emotions, thoughts, and behaviors and adjust their perspective on them. According to an article in the journal Medicine (Baltimore), cognitive behavioral therapy is one of the most effective psychiatric interventions for addressing chronic pain.5 CBT works to reduce chronic pain by adjusting how a person responses to physical sensations and behaviors that may contribute to the pain. For example, when a person starts to recognize pain or starts to feel anxious, depressed, or nervous due to the pain, CBT teaches relaxation techniques, distraction activities, mantras, or other options that help reduce the feelings of pain.
CBT understands that some people with a chronic pain syndrome, including complex regional pain syndrome (CRPS), have a variety of causes that contribute to the sensations of pain. Examples include immune system sensitivity, how a person senses and responds to pain, and responses from the central and peripheral nervous system. Fortunately, CBT is a common therapeutic approach. Many therapists can provide this therapy to help people learn how to identify and deal with their pain.
Hypnosis is a lot more than waving a watch back and forth. Hypnosis helps a person achieve a state of deep relaxation and comfort. In the treatment of chronic pain, hypnosis helps a person find a relaxing state when they feel pain or discomfort. Examples could include teaching a person to close their eyelids and take deep, full breaths to help themselves relax.6 Hypnotists call this practice “self-hypnosis.”
In a review of 13 studies on hypnosis, researchers concluded the following:6
Cancer Pain
Patients who used self-hypnosis along with group therapy participation experienced significant pain reductions when compared to those who participated in group therapy without self-hypnosis.
Lower Back Pain
Patients who use self-hypnosis to promote relaxation said they felt greater reductions in lower back pain when compared with patients who did not.
Arthritis Pain
A small study of patients with arthritis found those who participated in hypnosis had lower pain intensities compared to those who did not participate in hypnosis.
Fibromyalgia
Patients with fibromyalgia reported reductions in muscle pain, problems sleeping, and fatigue over the course of three months with the practice of self-hypnosis.
In most instances, self-hypnosis or hypnosis was more effective than no intervention at all in relieving pain.6 When used in coordination with other methods, such as cognitive-behavioral therapy, physical therapy, and over-the-counter medications, hypnosis helps to reduce chronic pain.
Meditation, or what some doctors call mindfulness meditation, is a practice that involves focusing on breathing while blocking out the surrounding environment.7 A study from the National Center for Complementary and Integrative Health asked patients to engage in meditation while also getting a magnetic resonance imaging (MRI) scan.7 Then, the researchers gave participants the medication naloxone (Narcan). This medicine blocks opioid receptors in the brain. Participants then engaged in meditation while they underwent another MRI.
At the end of the study, researchers found that people reported pain relief from meditation, even when they had taken naloxone to block opioid receptors. The researchers concluded that there are many other pathways in the body, other than opioid receptors, that could help relieve pain. This is promising for those who want to relieve pain using other approaches besides opioid pain relievers.
Pain skills workshops are workshops designed to help patients who experience chronic pain. You may see these workshops advertised as “Chronic Pain Self-Management Programs.” Some of the key services that these workshops provide include:
Exercises that can help with chronic pain and advice on how to pace one's self
Communication skills to teach how to best communicate with others about pain
Aspects of nutrition in pain management
Strategies to avoid common frustrations and concerns in those with chronic pain, such as fatigue, frustration, and problems sleeping
A study published in the journal Patient Education and Counseling studied the effects of a Chronic Pain Self-Management Program on 74 women and 13 men from Denmark who reported having chronic pain for more than ten years.8 The six sessions program focused on helping teach non-opioid methods to relieve pain.
The researchers followed up with the patients five months after completing the program.
They reported reductions in:
Pain
Depression
Anxiety
Worries about health
The researchers concluded that pain skills management could help a person better self-regulate pain.
Marijuana and cannabinoid (CBD) oil are a growing area of research for non-narcotic pain management. Currently, many states have approved the use of medical marijuana to reduce pain as well as stimulate appetite in people with chronic illnesses, such as cancer.
Marijuana contains a compound called tetrahydrocannabinol (THC) along with cannabinoids (CBD). CBD isn’t the same as THC. CBD isn’t psychoactive, meaning a person can’t get high from CBD alone. THC may have some pain-relieving effects, but it also causes mind-altering effects. For some people, this may include feelings of euphoria or being “high.”
Doctors think that CBD products act on a different set of pain receptors in the body known as the endocannabinoid receptors.9 By targeting these receptors, doctors think that some CBD products may help to relieve pain.
While many doctors think the field of marijuana and CBD for pain management has a lot of promise, they are cautious until there’s more research available. Currently, the U.S. Food and Drug Administration (FDA) hasn’t approved CBD as a medication. CBD is viewed as a supplement and is not regulated. Unfortunately, that means that it’s hard for people to know what kind of CBD or how much is actually in a product they buy.
A common misconception among Americans is that an organization regulates CBD. According to the American Society of Anesthesiologists, an estimated 40 percent of participants surveyed incorrectly believed that CBD found in medical marijuana and health food stores was FDA-approved. In reality, none of it is FDA-approved.

Even in states where marijuana is legal, doctors admit they can’t know what is in marijuana when they consider factors like pesticides, chemicals, and metals commonly found in marijuana.
While marijuana and CBD have a lot of promise in pain treatment, it’s important to remember that marijuana isn’t without its side effects. People with a history of addiction may want to consider alternative pain management practices rather than marijuana, as there is an increased risk of addictive behaviors with marijuana use. If you or a loved one is thinking about adding it to your overall pain management strategy, talk to your doctor first.
Different people experience pain in different ways. Two people can have the same surgery, with one person experiencing significant pain afterward, while the other quickly recovers. While the person who is still in pain isn’t at fault, this example shows how pain is a complicated issue that affects both the mind and body.
Some of the factors that doctors have found can make pain worse includes:
Sometimes fear and worry about pain can be as crippling as the pain itself. Treating anxiety has been shown to reduce reliance on pain medications.10 Using techniques such as distraction, creating a non-threatening medical environment, and helping patients learn how to deal with feelings of anxiety can be extremely helpful in addressing chronic pain.
While there is a time to rest an acute injury, not moving usually does more harm than good when it comes to chronic pain.11 When the body isn’t active, there is a tightening of muscles and tendons that can cause additional stress. Also, people who don’t engage in regular exercise are more likely to be obese. Carrying extra weight and not engaging in physical activity can increase pain, especially in the lower back and knees.
An estimated 61 percent of patients who take opioids and struggle with chronic pain experience major depression.10 The conditions are closely linked, and doctors think depression can cause chronic pain just as chronic pain can cause depression.
If you find you are struggling with depression, it’s important to talk to your doctor about your feelings. Some people end up accidentally self-medicating with opioids as a means to escape feelings of sadness and depression.10 Medications and therapies are available to help address feelings of depression. These strategies can decrease opioid use and address chronic pain more effectively. This isn’t always true for all people, but it can be worth trying if you struggle with chronic pain and depression.
Chronic pain and chronic stress are closely related. In fact, one article published in the journal Chronic Stress described the two conditions as “two sides of the same coin.” 12 Doctors believe that chronic stress can lead to a dysregulation in the brain. This means that too much or too little brain activity is experienced in response to stress. This can aggravate a number of conditions, including chronic pain in the body.
Stress is a common experience for many individuals, but daily and continued stress overwork, social interactions, health conditions, and chronic pain can impact a person’s overall perception of health and well-being. The results can be an increased pain experience. People who experience chronic pain should take steps to reduce overall stress levels, which can often lead to a mild to dramatic improvement in overall health and well-being.12
According to the National Sleep Foundation, pain, stress, and poor health are all connected.13 People with chronic pain sleep on average 42 minutes less than those who do not have chronic pain. Of those with chronic pain who report that it affects their sleep, 50 percent say their chronic pain also impacts their daily lives and work.
Doctors connect the ability to sleep well with good health. According to the National Sleep Foundation, people who report overall health and well-being at the highest levels sleep 18 to 23 minutes longer than people who report their health as good, fair, or poor.
Some tips to help people with chronic pain sleep well include:
Stopping caffeine consumption or refraining from consuming caffeine close to bedtime.
Refraining from drinking alcohol later in the evening.
Implementing a sleep schedule and bedtime routine.
Using relaxation techniques to help a person go to sleep, such as deep breathing and meditation before going to sleep.
Sleeping in a cool, dark, and comfortable location.
If opioids are being taken to relieve pain, caution should be used with any prescription or over-the-counter sleep aids. Always talk to your doctor before starting a sleep-promoting medication to see if the medicines could interact with current prescriptions.
In addition to sleep, nutrition is another key aspect that may affect overall health and wellbeing when dealing with chronic pain. Doctors have found that chronic inflammation in the body can contribute to pain. A person’s diet – good or bad – can affect the levels of inflammation in the body, thereby impacting pain levels.
Inflammation is essentially damage and irritation of healthy cells that can lead to pain. According to Harvard University, inflammation in the body can increase the likelihood of a number of health conditions, including diabetes, cancer, heart disease, and Alzheimer’s disease.14 Studies also indicate that a healthy diet can strengthen the immune system, while an unhealthy one can negatively affect it, causing inflammation in the body.
The solution can be to follow an anti-inflammatory diet. One of the best-known anti-inflammatory diets is the Mediterranean diet. This is a meal plan that includes a high amount of foods like berries, dark and leafy green vegetables, nut, whole grains, and legumes. These foods are high in inflammation fighters called antioxidants. Foods that have omega-3 fatty acids, such as fish, olive oil, and flaxseed oil may also help reduce inflammation and pain.
In addition to eating beneficial foods, it’s a good idea to avoid some foods that are known to contribute to inflammation. Examples include soda, foods with high-fructose corn syrup, processed meats, and foods that have refined carbohydrates, such as white pasta, white bread, and white rice. The good news is that following this meal plan not only reduces inflammation (and, therefore pain), it can also help improve overall health.
While a healthy diet and good sleep aren’t the only ways to improve chronic pain, they are lifestyle changes that can make a big difference. Taking steps to improve both can help to improve overall health.
Narcotic pain meds aren’t the only option when it comes to treating pain. While they may represent a beneficial treatment for some, taking steps to better respond to pain and increasing overall health through movement, diet, and better sleep can also help reduce pain.
If you aren’t quite sure where to start, talk to your doctor about your pain and overall health. You can discuss some of the interventions mentioned in this article and determine what will help you live better with your chronic pain. While you may not get the same immediate results that you might with a pain pill, non-opioid strategies can provide a safer and longer-lasting solution to managing chronic pain.
© Copyright 2024 Asana Recovery™ | All Rights Reserved | Privacy Policy
Asana Recovery
We firmly believe that the internet should be available and accessible to anyone, and are committed to providing a website that is accessible to the widest possible audience, regardless of circumstance and ability.
To fulfill this, we aim to adhere as strictly as possible to the World Wide Web Consortium’s (W3C) Web Content Accessibility Guidelines 2.1 (WCAG 2.1) at the AA level. These guidelines explain how to make web content accessible to people with a wide array of disabilities. Complying with those guidelines helps us ensure that the website is accessible to all people: blind people, people with motor impairments, visual impairment, cognitive disabilities, and more.
This website utilizes various technologies that are meant to make it as accessible as possible at all times. We utilize an accessibility interface that allows persons with specific disabilities to adjust the website’s UI (user interface) and design it to their personal needs.
Additionally, the website utilizes an AI-based application that runs in the background and optimizes its accessibility level constantly. This application remediates the website’s HTML, adapts Its functionality and behavior for screen-readers used by the blind users, and for keyboard functions used by individuals with motor impairments.
If you’ve found a malfunction or have ideas for improvement, we’ll be happy to hear from you. You can reach out to the website’s operators by using the following email
Our website implements the ARIA attributes (Accessible Rich Internet Applications) technique, alongside various different behavioral changes, to ensure blind users visiting with screen-readers are able to read, comprehend, and enjoy the website’s functions. As soon as a user with a screen-reader enters your site, they immediately receive a prompt to enter the Screen-Reader Profile so they can browse and operate your site effectively. Here’s how our website covers some of the most important screen-reader requirements, alongside console screenshots of code examples:
Screen-reader optimization: we run a background process that learns the website’s components from top to bottom, to ensure ongoing compliance even when updating the website. In this process, we provide screen-readers with meaningful data using the ARIA set of attributes. For example, we provide accurate form labels; descriptions for actionable icons (social media icons, search icons, cart icons, etc.); validation guidance for form inputs; element roles such as buttons, menus, modal dialogues (popups), and others. Additionally, the background process scans all the website’s images and provides an accurate and meaningful image-object-recognition-based description as an ALT (alternate text) tag for images that are not described. It will also extract texts that are embedded within the image, using an OCR (optical character recognition) technology. To turn on screen-reader adjustments at any time, users need only to press the Alt+1 keyboard combination. Screen-reader users also get automatic announcements to turn the Screen-reader mode on as soon as they enter the website.
These adjustments are compatible with all popular screen readers, including JAWS and NVDA.
Keyboard navigation optimization: The background process also adjusts the website’s HTML, and adds various behaviors using JavaScript code to make the website operable by the keyboard. This includes the ability to navigate the website using the Tab and Shift+Tab keys, operate dropdowns with the arrow keys, close them with Esc, trigger buttons and links using the Enter key, navigate between radio and checkbox elements using the arrow keys, and fill them in with the Spacebar or Enter key.Additionally, keyboard users will find quick-navigation and content-skip menus, available at any time by clicking Alt+1, or as the first elements of the site while navigating with the keyboard. The background process also handles triggered popups by moving the keyboard focus towards them as soon as they appear, and not allow the focus drift outside it.
Users can also use shortcuts such as “M” (menus), “H” (headings), “F” (forms), “B” (buttons), and “G” (graphics) to jump to specific elements.
We aim to support the widest array of browsers and assistive technologies as possible, so our users can choose the best fitting tools for them, with as few limitations as possible. Therefore, we have worked very hard to be able to support all major systems that comprise over 95% of the user market share including Google Chrome, Mozilla Firefox, Apple Safari, Opera and Microsoft Edge, JAWS and NVDA (screen readers).
Despite our very best efforts to allow anybody to adjust the website to their needs. There may still be pages or sections that are not fully accessible, are in the process of becoming accessible, or are lacking an adequate technological solution to make them accessible. Still, we are continually improving our accessibility, adding, updating and improving its options and features, and developing and adopting new technologies. All this is meant to reach the optimal level of accessibility, following technological advancements. For any assistance, please reach out to